Performance of the VA low vision visual functioning
questionnaire (VA LV VFQ)
Z. Ardickas, MA,1,2 J.P. Szlyk, Ph.D.,1,2 J. Stelmack, OD,2-4 R.W. Massof, Ph.D.,5 M. Kuzia, MS,1,2 T.R. Stelmack, OD,1,2,4 B.D. Wright, Ph.D.6 and the LVOS Group.
1Chicago
VA Health Care System/West Side, 2University of Illinois at Chicago, 3Hines
VA Blind Rehabilitation Center, 4Illinois College of Optometry, 5Johns Hopkins Wilmer Eye Institute, 6University
of Chicago.
Objectives: Our goal was to develop an instrument
that is sensitive to the effects of low vision rehabilitation.
Methods: Eighty-five patients (mean age=72.4
yrs), with a range of vision loss from mild impairment to total
blindness, from three sites (Hines Blind
Rehab Center, VA West Side VICTORS Program, Deicke Program) were recruited
and interviewed by phone prior to their rehab program admission. Our interview
guide contains 48-items on which the respondent is asked to rate (a) their
difficulty to perform a task, (b) whether their difficulty was related
to their vision, (c) whether they want training, and (d) how they currently
perform the task. Results: Data were analyzed with a Rasch rating scale
model. The difficulty question showed strong separation and high reliability
(S=4.04, R=0.94). The item ordering for the difficulty question (items
ranked from easiest to impossible) was highly correlated with the item
ordering for the following questions: (1) whether difficulty was related
to their vision (R=0.87), and (2) whether they wanted training (R=0.85).
Both of these correlations increased to 0.98 with the removal of 9 ineffective
items that included doing yard work and playing sports. The rankings for
the vision and the training questions were highly correlated, R=0.98 with
all 48 items.
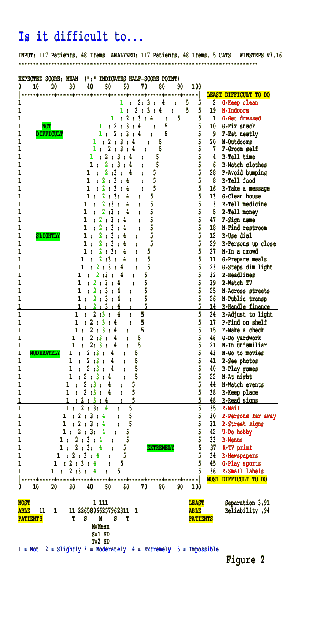
Figure: Item difficulty scale generated from
Rasch analysis showing the distribution of patient responses for those
items rated not difficult to impossible. Red highlighted items at the
top of the diagram indicate items rated as not difficult. Red highlighted
items at the bottom of the diagram indicate items rated as extremely difficult.
The vertical line drawn down the center of the diagram indicates the mean
measure for the patient group for each question. The item ordering for
the (subcomponent a) difficulty question was highly correlated with the
item ordering for (subcomponent b) whether difficulty was related to vision
(R=0.87). Also, the item ordering for the difficulty question was highly
correlated with the item ordering for (subcomponent c) whether they wanted
training (R=0.85).
Conclusions: The results show that the VA
LV VFQ is an effective instrument to measure vision difficulties in low
vision rehab patients in VA-based programs.
Funding Acknowledgment: This study was funded
by the Department of Veterans Affairs, Rehabilitation Research and Development
Service, project # O2086RA.
